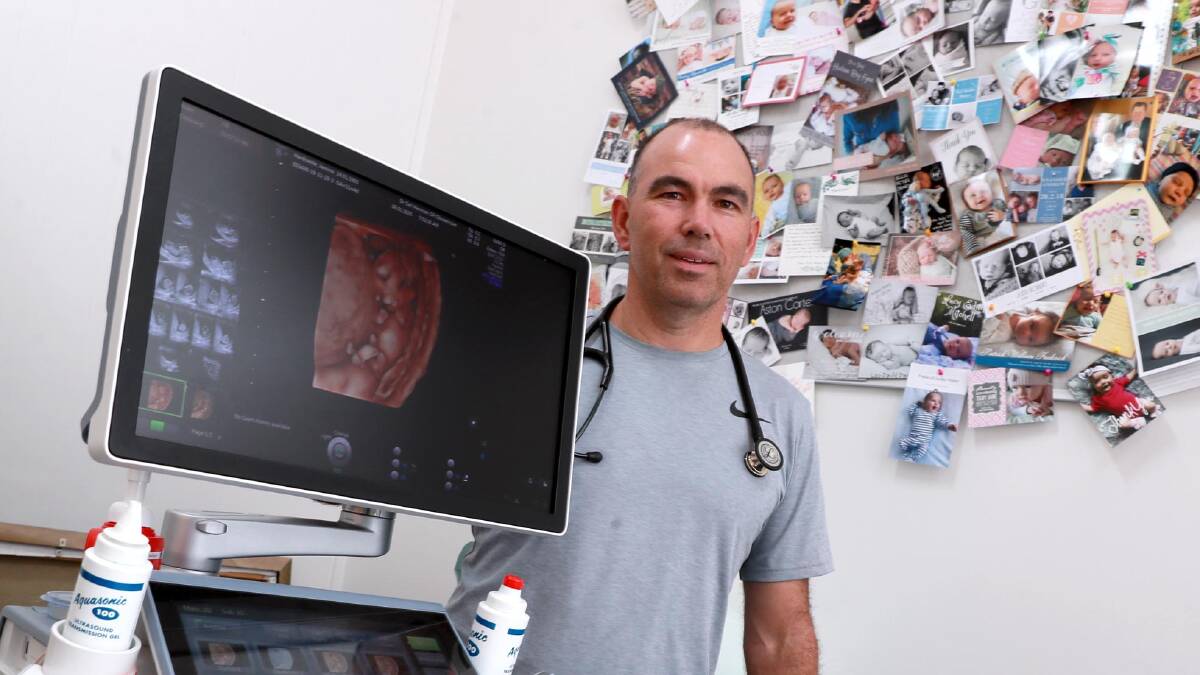
There are specific challenges to obtaining quality maternity care in the regions, Wagga doctors have told the state's birth trauma inquiry.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
GP obstetricians Trudi Beck and Carl Henman both addressed the inquiry and echoed echoed the arguments of experts who spoke in Sydney on the importance of continuity of care and informed consent.
Successive inquiries into the public health system have found a "postcode lottery" when it comes to obtaining quality care of any kind.
Witnesses before the Wagga hearing of the inquiry on Tuesday morning reported feeling like they were being passed around by medical staff, who weren't across their pregnancy.
Dr Henman said sometimes decisions are made out of fear by doctors concerned about lacking the staff for an emergency intervention if it is needed.
He said the practice of obtaining consent during the birthing process "made a mockery of the idea of consent".
"Reading the submissions, I thought to myself I could see it from the doctors perspective, that it looked like it was turning south quickly, and they wanted to know for example what position the head was in," he said.
"The consent in that particular setting is not ideal consent, but I think if you had explained to that lady prior to labour that this might have to occur for these reasons she's a bit less likely to say she felt assaulted."
Dr Beck is in a unique position as someone who works in both a private pregnancy clinic and in the public system.
She offered insights about the working relationships between different medical professional. She told the inquiry doctors in her position are often disempowered when patients are referred to hospital, breaking the continuity of their care.
"We have been used to being the point of reference for our patients over a long period of time. I hope over that time we've developed trusting and mutually caring relationships," she said.
"When we refer the patient to the hospital, it's almost as though the patient then belongs to the hospital.
"My belief from working in the system is safety and minimisation of risk has come at the extent of true collaborative care. I can't criticise that because I understand it's well-intentioned, but I believe that the patient experience with that may look like fragmentation."
Following on from individual testimonies this morning, The inquiry asked how continuity of care could be improved.
Both doctors spoke about the importance of individualised care to help women feel safe, and the importance of trust relationships built over time.
Dr Henman said a number of witnesses had conflated interdisciplinary care with continuity of care.
"The more providers you put into any care, the more likely you are to create fragmentation," he said.
"Most patient birth experiences are good ones, conducted in healthcare system we're very lucky to have available. That doesn't mean it can't be approved.
"Much is made of multi-disciplinary teams ... they are by their very nature leading to fragmentary care - exactly the opposite of what these women need.
Birth trauma is something unique to every individual, and the inquiry has heard since the first hearing about the importance of informed consent being central to avoiding birth trauma.
Dr Beck said she had observed women who've had a "wild ride" of a birth that have come out untraumatised.
She said clear communication during the antenatal process about the possible complications, and the merits and dangers of different interventions.
"Consent's not just having a NSW Health checklist," she said.
"It's saying this is the fork in the road we're at, this is my clinical opinion, what I my training would lead me to believe, these are the pros and cons of each - what do you think?
Dr Henman agreed. He said this is why continuity of care that produces relationships of trust between doctors and patients is so important.
"It's as simple sometimes as asking 'what's your expectation?'" he said.
"I think establishing a system where those types of things can be discussed before would be a reasonable way to go about that.
"Without that education, we shouldn't necessarily assume why a woman should know something [an expectation] might be reasonable.
"It comes back to having a trusted care provider you can ask those questions of, or knows you and can raise those questions appropriately.
Dr Beck said a better understanding of "patient-centred communication would help doctors offer better care", something she offered midwives are generally better at.
She said she had never been given explicit training in informed consent.
"It's not what you say, it's how you say it," Dr Beck said.
"When you look at how far all practices have come in the last few decades, incremental change has to occurred, and picking each other up when we say something to our patients, recognising there's a power differential and how do we be humble clinicians?
"It's my number one recommendation significant resources should be put into promoting, encouraging and facilitating longitudinal models of care under a trusted lead carer."
Committee member Mark Banasiak asked about the challenges of addressing the problem at scale, acknowledging the limitations of the health system.
Dr Beck said this is not necessarily an expensive problem to solve, but requires greater attention to be paid to language, and the culture within the health system.
"The birth and the pregnancy belongs to the woman. The birth and pregnancy does not belong to NSW Health," she said.
"If we put that out there, we automatically default to consent.
"It's not the guidelines that are the problem - it's the way we implement the guidelines."