New figures show that the overall rate of HIV transmission in Australia is dropping. Sally-Anne Brennan, a clinical nurse specialist, has been working in the area of sexual health in Wagga for two decades.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
Sally-Anne, it is 21018. Where are we with HIV?
HIV infections have declined in NSW over the last decade. NSW Health is working towards the goal that by 2020, new HIV transmissions will be virtually eliminated.
To achieve that, we want to encourage HIV testing and if people are newly diagnosed that they start therapy as soon as possible. This will ensure better health outcomes for the individual and also reduce the risk of HIV transmission in the community.
What would you most like people to know about HIV?
The key is to know your HIV status, particularly if you are at increased risk of HIV. If you have never had an HIV screen or have had at-risk behaviours, now is a perfect time to know your status.
GPs or a specialist sexual health services provide HIV screening, which is just a simple blood test.
We encourage people to think about their sexual health and their general well-being.
Are we still living with the myths about who is affected or have we moved past that?
Thankfully we have moved past that. Anyone can be at risk of acquiring HIV if they have unprotected sex or share injecting equipment after someone else.
Last year we saw that one in five HIV notifications were in the heterosexual community. People who come from a country where HIV is common or have had sex when travelling in a country where HIV is common should have a HIV test.
Are we getting the safe sex message or have we become a bit slack?
The message is always there. Condoms provide the best protection regarding HIV and STIs.
We encourage people to think about their sexual health and their general well-being. Using condoms, having regular testing and, if they are injecting, making sure they have access to clean equipment is advised.
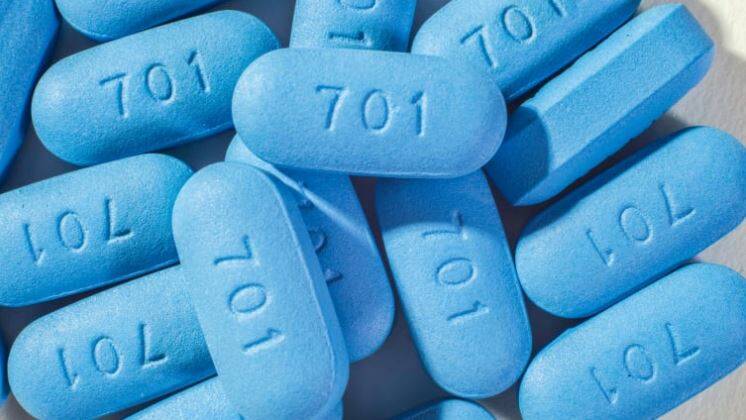
Where are we with treatments like PrEP? Are they making a difference?
I think this is a very exciting time in terms of HIV prevention. PrEP is basically pre-exposure prophylaxis, so it’s for HIV-negative adults who are at high risk and ongoing risk for HIV.
What it entails is going along to their GP, having an assessment for PrEP. If the individual meets the criteria, GPs provide a prescription as it is now listed on the PBS. Community pharmacies can dispense PrEP prescriptions.
I’m encouraging people, even though they are using a prevention medication, to use condoms because PrEP doesn’t prevent other infections such as syphilis, chlamydia and gonorrhoea. It will only prevent acquiring HIV.
The Australasian Society for HIV, Viral Hepatitis and Sexual Health Medicine is about to host a major conference in Sydney about HIV?
This is a fantastic opportunity for clinicians, researchers and people with an interest in the field come together to share their knowledge. It’s about planning for the future as well, making sure we’re doing best practice when it comes to looking after the health people living with HIV.
You touched on some of the other sexual transmitted infections that are around. What would you like people to know about those?
You can have an infection without having any signs or symptoms. The only way individuals really will know is if you have a test. Screening for chlamydia and gonorrhoea is just a simple urine test.
It’s really important that when people go to their doctors, they are able to discuss their sexual history, so that the most appropriate screening can be done.
Are people getting more confident about going to their GPs and talking about these issues?
I think they are. We live in a very social media-driven world these days. Many messages do come across through social media, but also it’s about people taking time for themselves and making sure they’ve booked for a screening, given that some STIs are without symptoms.
Timely access to STI testing and treatment is vital when thinking about sexual health.

On a more personal note, how did you come to specialise in sexual health?
It’s been a great privilege to work in sexual health for 22 years. Seeing the wonderful advances in HIV care means that people living with HIV in our community and around the world have better health outcomes.
People who are newly diagnosed with HIV and on therapy will have “well lives” with normal life expectancy. HIV is a chronic, manageable condition. But very importantly HIV can be prevented, so we need to make sure people have access screening and prevention opportunities.
It’s rewarding to play a role in caring for people living with HIV, normalising life, having families, engaging with the community and workplaces, doing all the things people like to do.
We know for people living with HIV, the specialised medication reduces the HIV viral load, this means they will be well and it also means with an undetectable viral load there is no risk of transmitting the virus.
When you look back, say 20 years, it must astound you that treatments have improved so much?
It’s amazing to see the continued advancements in HIV medication. It’s essential that people living with HIV engage with specialised sexual health services and GPs to ensure they have the best health outcomes.
Read more: