Let’s be completely honest. Nobody wants to have to stay in hospital.
Subscribe now for unlimited access.
or signup to continue reading
For people who are seriously ill, there is obviously a great deal of comfort – and medical necessity – in being within seconds of health professionals.
But what if your condition is not acute? What if, for example, your recovery is well advanced and you’d be able to be at home, were it not for the need for regular checks by nurses or physiotherapy, for example?
That’s where the Hospital in the Home service at Wagga Base Hospital is tipping traditional ideas of care on their ear.
Hospital in the Home is about as far as it is possible to get from those images of Victorian-era hospitals filled with patients in row after row of single beds and nurses in starched white aprons.
The program’s goal is primarily two-fold: It helps to ensure hospitals beds are freed up and acknowledges that many people are much happier when they are able to recuperate in their own homes.

Instead of facing a stint in an unfamiliar hospital, patients are able to stay at home, but still be cared for by health professionals.
Nurses, pharmacists, physiotherapists and dietitians are all part of the service, which has treated almost 300 patients in just six months, and those numbers are rising.
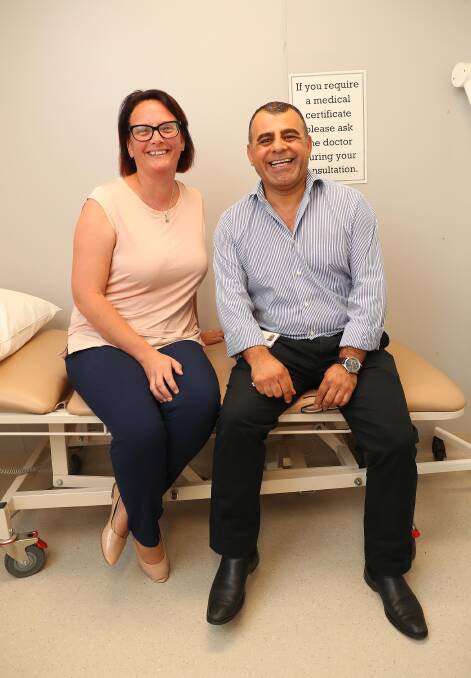
Rashid Samad, the nurse unit manager of the ambulatory care service, is enthusiastic about this evolution in health care.
He said patients who were assessed as being “acute” and “sub-acute” were primarily those considered for the program.
“Not every patient is happy in hospital. Some are much happier being treated in their own home, Mr Samad said.
One of the big advantages of the HITH program is a continuity of care. The team that treated the patient while they are in hospital continues to see the them after they go home.
Mr Samad said this continuity of care was a priority, and each patient went home with a detailed care plan.
“If someone comes to give you your antibiotics at 1pm today, someone will come and give you your antibiotics at 1pm tomorrow,” he said.
The service operates seven days a week, between 7am and 9.30pm, and within a radius of 30-kilometres of the hospital.
“We can have people who can stay in hospital for two weeks, six weeks, even a couple of months,” Mr Samad said.

“Who wants to be in hospital for six weeks to have antibiotics?
“This is an alternative for anything that could be safely administered at home.”
Mr Samad said there were differences between the HITH’s model of care and the more-often recognised services offered by community nurses.
The most obvious is that the HITH services allow patients to remain under the care of the same medical teams who treated them during a hospital stay and were already familiar with their treatment needs.
Naturally, there is no such thing as a “typical” patient, but Mr Samad said there were people whose conditions were more often suitable for the program.
”People who are being treated for something like cellulitis or who have a small fracture, people who are being treated with blood thinning medications who require regular injections or who have respiratory conditions are often included,” he said.
“Doctors conduct reviews at least once a week, while nursing staff do reviews at least once a day.
“People can also come in to the clinic for review.”
It’s not just patients with one-off injuries or illnesses who can make use of the HITH program.
Mr Samad said there are patients with long-term conditions that would previously have necessitated lengthy stays in a ward, who are able to at least reduce the amount of time they’re in hospital by using the service.
“Imagine if you were looking at staying in hospital for several weeks, but instead were given the option to spend at least some of that time being treated from home instead,” he said.
“People are just happier when they are able to go home.
“Nothing really changes, but you’re just not hearing those noises from the hospital.
“You may have a canula in, but you can cook your own meal while you’re waiting for the nurse to come.”
With the truism of there being exceptions to every rule, the program which aims at helping people stay at home, also offers treatments on-site for a particular group of patients.
These patients are those who require regular, lengthy, treatments using IV medications.
So while Helen Sargent still has to come into the hospital, being able to have her medication administered by staff working from the HITH premises keeps her out of the hospital wards.
Ms Sargent’s medication is administered by IV every three weeks in a process that can take up to five hours.
“It really is a godsend for me,” she said.
“At least this way, you can come in and have treatment, then avoid being in hospital. My blood pressure goes up just knowing I have to come in here. Imagine what it would be like if I had to be admitted.
“But this way, I’m not clogging up the hospital. It’s keeping a bed free for the people who really need it.”
As Wagga Base is transformed with the construction of the new main hospital and ancillary buildings, HITH is to receive a new permanent location in stage three of the project.
For now, staff have been moved out as their old digs are demolished in preparation for the new building work and are operating from temporary buildings.
“Health care has changed,” Mr Samad said.
“It is thinking beyond just conventional hospital kind of things.
“This is a really good service.
“Just imagine being able to stay in your own home and being treated by nurses.
“I feel happy that in six months, we have been able to provide for 300 patients.”
“That’s nearly 300 people who have been able to leave hospital earlier or avoid a hospital stay altogether.”