
Emily Day is a placenta encapsulation specialist - and while that may sound strange to some, what led her towards this unique pursuit is far more common than many would wish to believe.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
Her story begins in 2018 upon discovering that she and her husband, Braden, were pregnant with their first child. Like many first-time parents, feelings of excitement and fear followed.
Although she was a nurse at Wagga Base Hospital, giving birth to babies was something she was "not so trained in".
But one thing was for sure; she was going to do anything she could to "avoid a traumatic birth experience".
"Unnecessary interventions can cause a lot of harm, and mothers and babies can come out of that experience significantly worse for wear," Mrs Day said.
"I was aware of that going into my first pregnancy."
A plan was also drawn up to provide Mrs Day with the water birth she wanted after her dreams of a home birth were shattered by a lack of assistance for such a thing within the region.
Even then, after a "beautiful and easy-going pregnancy", she was admitted to hospital at 38 weeks due to her rising blood pressure and her pregnancy was declared "high-risk" by medical staff.
Despite lengthy testing showing no signs of preeclampsia, a potentially dangerous pregnancy complication characterised by high blood pressure, the label stuck.
"The hospital slapped that tag on me that I was high risk for no rhyme or reason," she said.
"Because I was labelled as high risk I wasn't allowed to have the water birth that I wanted."
As a nurse, Mrs Day was confident in monitoring her own blood pressure in the comfort of her own home.
As a pregnant mother, she knew better than anyone the signs that her baby was in distress.
"I was very stressed being in the hospital," she said.
"Working within the public health system as a nurse and caring for sick people, I thought to myself that I didn't really want to be there because I actually wasn't sick.
"I was birthing a baby, and that is not an illness."
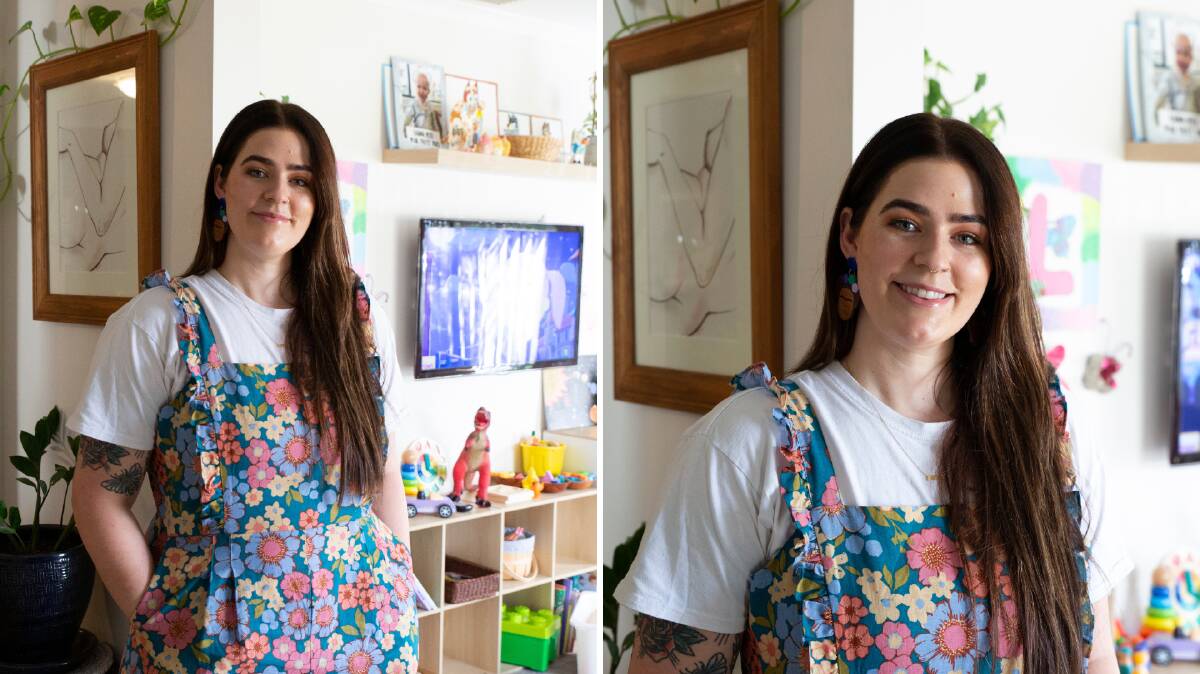
Although scheduled to be induced, Mrs Day's water broke earlier than expected, which came with a sigh of relief.
But while her recollection of what led up to this all-important moment had been vivid, the birth of her first child is something she struggles to recall.
"I was given a shot of morphine to try and help keep on top of the contractions," she said.
"The midwife told me because I was a first-time mother that I shouldn't be giving birth within the next four hours."
But, within those four hours, Laina Audrey was born "floppy", "blue" and silent.
The child "thankfully" did not require resuscitation, however, the deep, third-degree tear Mrs Day obtained had to be treated with another form of pain relief.
"I was passing out," she said. "The four times I had my baby in my arms doing skin to skin with me, I don't remember a single minute of it - those precious golden hours.
"I still ask my husband to this day to recount those moments for me."
According to Mrs Day, the hospital was understaffed, and due to Laina's "quick" entrance into the world, she didn't have time to release the mucus in her lungs.
Within the first 45 minutes of transferring from the birthing suite, the new mum hit the emergency button.
MOTHER'S DAY 2022:
"Six midwives came running in, grabbed her from my arms, tipped her over to release a huge piece of mucus," she said.
"We were just in absolute survival mode."
This happened six more times within the following 24 hours.
"I was scolded for pressing the emergency button one too many times for them to come in and assist us in dislodging that mucus."
Four days later, Mrs Day's milk came, but Laina would not feed.
"One of the midwives even stood there, crossed her arms in the middle of the night and said, 'I don't know what more you want me to do', and I just burst into tears."
Mrs Day barely slept during the first nine days of returning home out of fear that her baby might choke in her sleep.
Laina was still not feeding well, and fast forward seven weeks, no GP, midwife or lactation specialist could provide a reason as to why.
At this point, the child was "tiny", "screaming" and never slept more than an hour at a time.
Feeling "utterly alone" while her husband travelled for work, Mrs Day had reached her breaking point.
"I no longer wanted to live, because it was just too excruciating," she said.
"My body was absolutely exhausted, depleted and tired. Postnatal depression and anxiety were getting the better of me.
"I ended up self-referring down to a Laser Clinic in Wodonga and they quite literally saved my life."
The clinic diagnosed Laina with severe tongue and lip tie which makes feeding at the breast or with a bottle impossible. The baby was starving as her lips could not properly form around the nipple and gain that suction required to feed.
Reflecting upon all that had happened leading up to that eight-week point, Mrs Day felt failed by the health system.
"I believe I tried to set myself up as best I could, but I was failed... I was not listened to," she said.
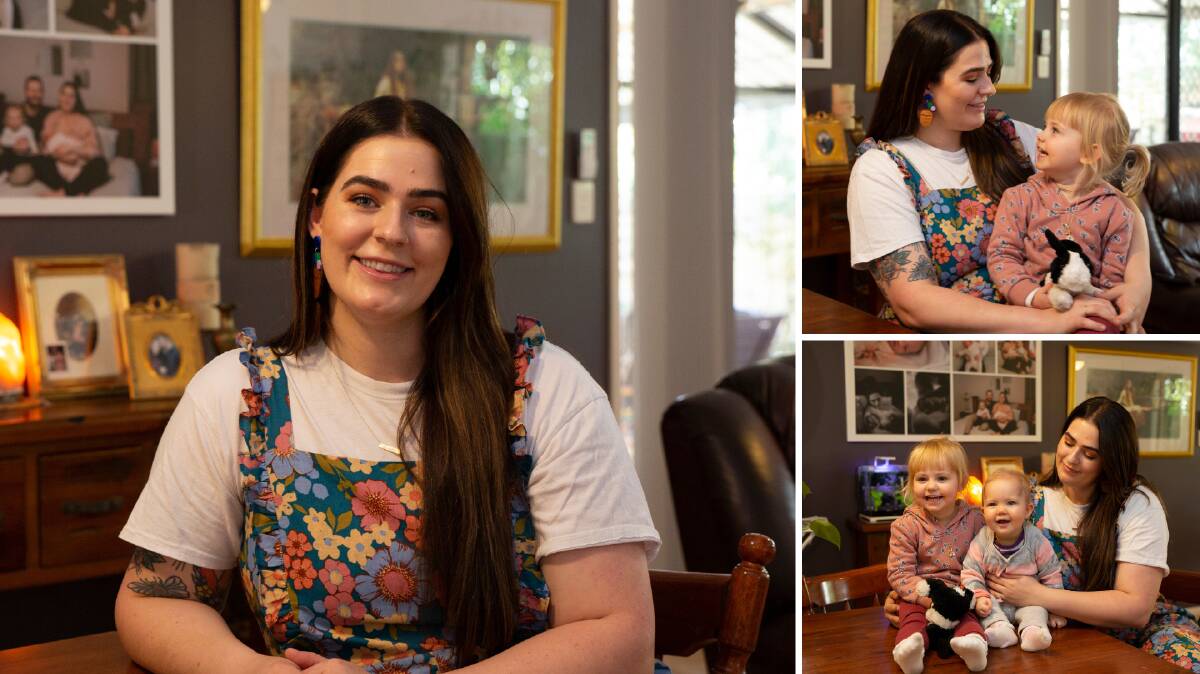
Fast-forward again to 2021, and the home birth of her second daughter Dulcie changed everything.
Not only was her "peaceful" entrance into the world less painful, but it enabled Mrs Day to heal from her previous birth trauma.
The mother-of-two began using her compelling story to encourage other women to take control of their pregnancies and combat the stigmas associated with postnatal depression.
"Mothers on Instagram and Facebook will post pictures of their babies at the park or with them while having coffees with their girlfriends in the first few weeks because their baby's sleeping well and happy," she said.
"But that is only a reality for just a very small, small percentage of women.
"Behind the scenes of those perfect Instagram posts, women are suffering from postnatal depression, postnatal anxiety, and a lack of support."
A lack of modern postpartum services catering to the needs of pregnant women within regional Australia is something that Mrs Day also made a direct step towards tackling.
In November last year, she opened Dulcie Lane Placenta Encapsulation & Postpartum Essentials, a business catering to pregnant women across the Riverina.
"I'd come up with this crazy idea at two weeks postpartum while I was resting in bed that I would do some study to become a certified placenta encapsulation specialist," she said.
Based on the traditional Chinese theory, the women's placenta is treated and served like food - washed, dehydrated and ground into a fine powder for the mother to consume as a pill-like capsule.

Placenta encapsulation continues to rise in popularity throughout western countries to support women through their fourth trimester - the 12-week period after childbirth where mothers can experience afterbirth pains, tenderness, bleeding, hormonal withdrawal, issues breastfeeding and other side effects.
When Mrs Day sought out this service during her first pregnancy, her husband was tasked with hand-delivering her placenta to a specialist, hours away in Victoria.
Knowing that distance is not an option for other local women, she wanted to fill the hole in the growing market.
"[The placenta] is the only organ in our body that is temporary ... you can't get that back, so missing out on these opportunities just is absolutely devastating."
The business has also provided her with another platform to share her incredible yet awfully common story with expecting mothers, hoping that one day the brutal realities of motherhood can be discussed openly.
If reading this story impacted you in anyway, please contact: Lifeline on 13 11 14, Suicide Call Back Service on 1300 659 467, or beyondblue on 1300 22 4636.
Our journalists work hard to provide local, up-to-date news to the community. This is how you can continue to access our trusted content:
- Download our app from the Apple Store or Google Play
- Bookmark dailyadvertiser.com.au
- Follow us on Twitter
- Follow us on Instagram
- Follow us on Google News
- Make sure you are signed up for our breaking and regular headlines newsletters


